Overview of keratoconus
Keratoconus is an eye condition that affects the shape of the cornea, causing vision loss. Our vision relies on our corneas, which are transparent barriers at the front of the eye. In people with keratoconus, the cornea’s structure changes over time, becoming cone-shaped and thinning. This affects the eye’s ability to focus, leading to visual impairments and light sensitivity.
The exact cause of keratoconus has not been identified, but it is thought that both environmental and genetic factors may play a role. People with a family history of keratoconus, other genetic conditions and allergies are more likely of being diagnosed. It is also thought that excessive and frequent eye rubbing may be a contributing factor.
Compared to eye conditions like myopia, keratoconus is rare, with approximately 1 in 2000 people being affected. It most commonly begins in the teenage years and develops gradually. In many cases, the condition will progress for 10 to 15 years, at which point its effects will stabilise.
Symptoms of keratoconus
Keratoconus presents a variety of symptoms depending on the severity of the condition and the individual case. Changes to the shape of the cornea lead to irregular astigmatism, which is a refractive error of the eye. This causes the vision loss and distortions that are typical of keratoconus.
The first symptoms you are likely to notice are blurry or distorted vision. This may come in the form of double-vision, and straight lines appearing curved or wavyPeople with keratoconus often experience frequent changes in their vision and symptoms and may have to regularly update their prescription glasses or contact lenses. As the condition progresses, the eyes become more astigmatic, meaning that Gas Rigid Permeable lenses may be needed to replace glasses or regular contact lenses.
Another common symptom is light sensitivity, which is especially prevalent as the condition becomes more severe. Sensitivity to bright light may cause difficulties when driving at night, with some people experiencing halos, light streaks, and glare.
Seeing an eye doctor or optometrist is advisable if you experience a rapid decrease in vision. Keratoconus presents in different ways and having a professional examination is the best way to catch a developing eye condition.
Diagnosis of keratoconus
Keratoconus can be diagnosed during a comprehensive eye exam, which will include a series of tests and questions about your eye health and family history of eye conditions. To make a positive diagnosis of keratoconus, optometrists will predominantly look at the thickness and shape of the cornea. The main tests used to do this are:
In this test, a specialised kind of microscope is used to examine the eye while a beam of vertical light is passed over it. This allows an optometrist to assess the structure of the cornea. Many different signs may lead to a diagnosis of keratoconus but optometrists are especially looking for corneal thinning and a change of shape in the cornea.
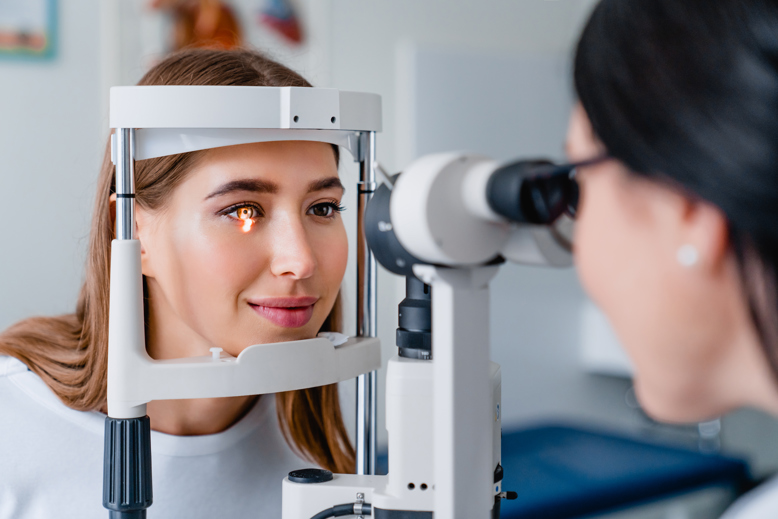
Keratometry is the measurement of corneal curvature. During a keratometry test, an optometrist place a ring in front of the eye that is reflected in the cornea. By measuring the reflection, they can assess the shape of the cornea.
Also known as Corneal Topography, this process captures the shape of the cornea to create something that resembles a topographical map. The map can then be used to identify the characteristic cone shape of corneas affected by keratoconus.
Pachymetry refers to measurements of the thickness of the cornea. A pachymetry test can be carried out using ultrasound technology or ocular coherence tomography (OCT). It is necessary to measure the thickness of the cornea before certain kinds of eye surgery, but it also helps optometrists diagnose keratoconus and determine how far the condition has progressed.
Treatment options for keratoconus
Treatments for keratoconus vary depending on the severity of the condition. The goal of keratoconus treatment is to help patients manage their vision loss and to stop or slow down the rate at which the condition is progressing.
To manage vision loss and distortion in the early stages of the disease, simple soft lenses and prescription glasses can be used, though they may require frequent updates because of the changing shape of the eyes. As the condition progresses, the eyes become more astigmatic meaning that Rigid Gas Permeable lenses and other speci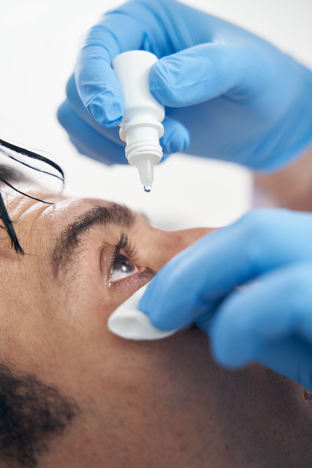
Corneal Cross-Linking is a treatment designed to strengthen the corneas and slow down or prevent the progression of the disease. Using medicated eye drops and UV light, fibres in the cornea are interlinked, which can help to stabilise its shape. This has been shown to be particularly effective in slowing down the progression of keratoconus.
Intacs are a minimally-invasive procedure to treat moderate keratoconus. By inserting Intacs within the tissue of the corneas, they can reshape them minimising vision loss and helping to prevent the condition from getting worse.
Conductive Keratoplasty is an emerging non-invasive treatment. The procedure uses radio frequency to reshape the cornea and correct the irregular astigmatism associated with keratoconus, which helps to improve the patient’s vision loss.
If keratoconus becomes very severe or is only diagnosed at a late stage, a corneal transplant may be necessary to treat it. By replacing the cornea with a healthy one supplied by a donor, the vision loss caused by the condition can be reduced. As with any surgery, the procedure comes with risks including rejection of the donor tissue and infection. This is why a corneal transplant is only considered when the condition is especially severe or does not respond to other treatment methods.
Managing Vision Loss with Keratoconus
As with many eye diseases, keratoconus leads to challenges in personal and professional life. The vision loss, distortions and light sensitivity caused by the condition can make activities like reading and driving difficult or impossible. Other symptoms like headaches, eye irritation and dryness can also cause difficulties in everyday life. Nevertheless, with the right products and professional support, people with keratoconus can effectively manage their condition and minimise its effects on their everyday lives.
The vision loss associated with keratoconus ranges from mild blurring in the early stages to an impairment of the eye’s ability to focus. Visual distortions can make reading extremely difficult, with the text appearing wavy, tilted or doubled. Light sensitivity is another symptom that people with keratoconus may experience. This not only causes discomfort but visual impairment that can affect a person’s ability to perform everyday tasks. This is why people with keratoconus often struggle with driving at night. The glare and halos caused by bright lights limit your ability to see, which leads to an increased risk of accidents.
Using specialised contact lenses or glasses helps to manage the vision loss caused by keratoconus and reduces other symptoms including light sensitivity. The most severe complications and symptoms of keratoconus are also quite rare. With expert help from an optometrist, patients can find a way to manage their condition and minimise its effect on their occupation and daily life.
Surgical Options for Keratoconus
Surgical options are considered for keratoconus when the condition is more advanced and cannot be effectively managed through other treatment options. Indications for surgery include corneal scarring, the cornea becoming extremely thin and vision loss that cannot be corrected with contact lenses or glasses. The available options depend on the severity of the condition and the individual needs of the patient.
A minimally invasive surgical option for moderate keratoconus is Intacs. Clear plastic implants are surgically applied within the cornea, reshaping it and improving vision. Intacs are also designed to allow contact lenses to be used more effectively, so you can continue to manage vision loss over time.
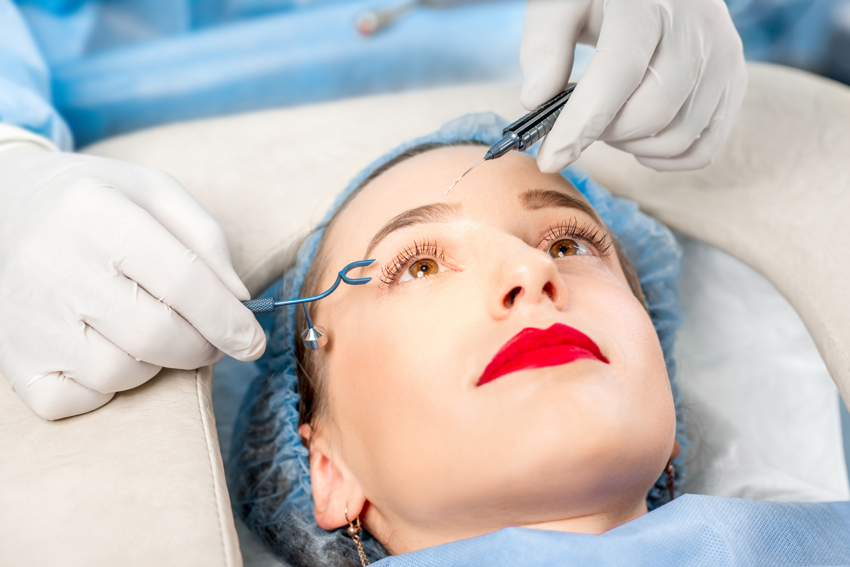
In cases where the cornea is badly scarred or extremely thin, a corneal transplant may be advised. The surgery involves removing the damaged part of the cornea and replacing it with healthy tissue from a donor. There are partial and full-thickness options for corneal transplants, which are recommended based on each specific case.
Surgical options carry greater risks than other treatments or management options. With corneal transplants, there is a risk that the donor tissue will be rejected and there is a possibility of infection. The surgery also requires a recovery time of 2 to 3 weeks.
The majority of surgeries, however, provide positive results and can make a huge difference to people with keratoconus. Both corneal transplants and Intacs can radically improve vision and reduce the other symptoms of keratoconus, allowing people with the condition to improve their quality of life.





